Life is so SPINE chillingly beautiful!
Brew with bones as you enjoy this special SPINE chilling issue
A stitch in time…. #NeoArmory
How difficult can placing a stitch be? Depends on the tear. Simple enough? Not exactly. It’s a microscopic surgery with the incision less than 2 inches, you are at least 3-4 inches deep, you are already a few hours into the surgery, the tear is a few mm in length and now for the best part, it is on the dura. The closure needs to be watertight. We can feel some spine surgeons moving in their seats reading this.
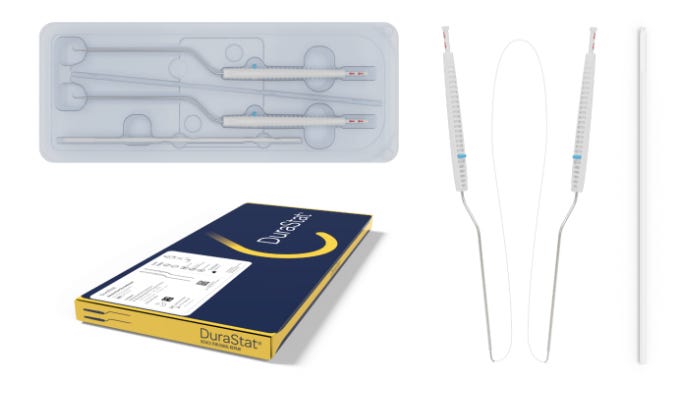
Introducing “DURASTAT”, a patented suture design with a Nerve hook deployer that allows tent the Dura up before passing the needle. This prevents Nerve entrapment under the suture. The system is preloaded with a 24” 5-0 PTFE suture. This has a blunt round needle with the same diameter as the suture and provides water-tight closure by avoiding needle tract leaks.
The bayonet handle allows better visualization. This is extremely useful when using tubular retractors. Otherwise, the repair would involve extending exposure to accommodate instruments. The ability to achieve water-tight closure without extending the incision can allow early ambulation and better outcome. So having it as a part of your spine surgical armory could be useful.
Flex it like Janz: #FromTheHistory
There is no better word to attribute Dr. Karin Büttner-Janz other than flexibility. Well, Genius may be the next better word. She is a gymnast par excellence. From winning the East German Athlete of the year award at the tender age of 15, she rose, rose, and rose. She had a whooping 7 Olympic medals and 3 world championship medals at the end of her gymnastic career. Her reputation was such that she has an uneven bar gymnastic event named after her – the Janz Salto.
But little did anyone around her know that her best is yet to come. Dr. Janz started her Orthopaedic career at the Charité hospital. Soon she started working on devices to improve mobility and flexibility in patients with disc diseases. She was wary of fusions. She developed the first artificial disc with her colleague Dr. Kurt Schellnack, known as the Charité disc. The device in its third generation now is still being widely used. She was the president of the International Society for advancement in spine surgery. No wonder she was also inducted into the International Gymnastics Hall of fame.
Patching it up: #SurgicalPearl
Incidental durotomy during elective spine surgery? Don’t you worry. Xiong et al propose a simple technique of patching it up using an epidural blood patch.
Repair the durotomy defect as usual.
Permit the fresh blood to pool from the surrounding surgical field directly onto the durotomy site. A scalpel blade was used to incise the lumbar musculature to obtain an adequate volume of blood.
The clot formed was blotted and dried by gentle dabbing with a gauze sponge to confirm a firm, dry accumulation.
After 3-5 minutes, the integrity of the clot was tested by probing and its adherence to the underlying dura is confirmed.
The integrity of the epidural blood patch is also checked with a Valsalva maneuver to a pressure of 40 mm Hg ensuring there was no persistent CSF leak;
In the authors’ experience, persistent dural leak did not interfere with clot formation, even in complex durotomies. Mind you! Incidental durotomy is the second most common cause of medical malpractice claims following spine surgery. This method is allergy free and cost-effective.
Know to patch things up.
Golden hour in spine trauma - #MostCited
Golden hour in spine truama has been an elusive question.
Lets look at the recent evidence by Sterner et al.
The authors evaluated the neurological outcomes of tSCI patients undergoing early versus late surgical decompression. They also noted the impact of transport time on neurological recovery.
Patients with transport time < 6 hours were associated with significantly (p=0.004) higher conversion of ASIA grade to less impaired states.
Patients who received decompression within 0 to 12 hours were associated with significantly (p<0.0001) higher average improvements in ASIA grade.
Faster transport and surgery at the earliest might become the norm in spine trauma care.
Stem cells, stem cells everywhere - challenging gold standards then n there #Intrails
The gold standard for spinal fusion is with an autologous bone graft. MSCs are challenging the gold standards of many orthopedic procedures. Spinal fusions are no exceptions. Blanco et al are conducting a long-term clinical trial to study the safety, feasibility, and potential clinical efficacy of autologous MSCs embedded with tricalcium phosphate as a therapeutic alternative to bone graft during posterolateral spine fusion.
There is no graft site morbidity in the procedure. The early results are quite promising. 80% of patients have achieved lumbar fusion radiologically at the end of the one-year follow-up with no adverse effects.
Stem cells, stem cells everywhere - challenging gold standards then n there
Answer to Last month’s question:
Medial meniscus bucket handle tear
Check out these cool events lining up:
POSNA Annual Meeting Nashville 2023 Nashville, United States - 25 April 2023 to 29 April 2023
2023 World Congress on Osteoporosis, Osteoarthritis and Musculoskeletal Diseases Barcelona, Spain - 04 May 2023 to 07 May 2023
The 96th Annual Meeting of the Japanese Orthopaedic Association Yokohama, Japan 11 May 2023 to 14 May 2023
Question of the month:
On the oblique view of the lumbar spine, what does the arrow pointing towards indicate?
Watch out for our next issue to know the answer. Happy year-end guys.